The heel (also called the calcaneus) is the largest bone within the foot and is often prone to injury due to overuse. Depending on the severity of the condition, heel pain may range from mild to disabling.
There are many causes of heel pain, such as by trauma, inflammation, or a systemic disease such as rheumatoid arthritis. This post highlights a common condition that leads to heel pain – plantar fasciitis.
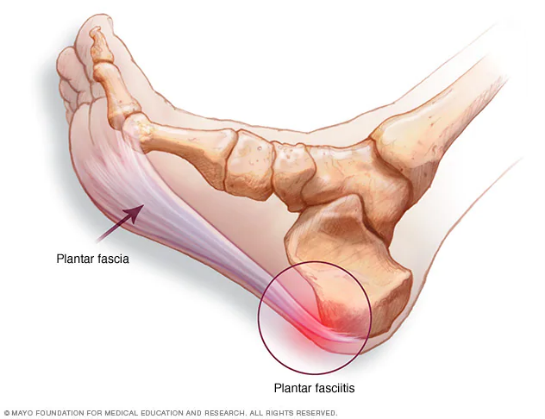
Plantar fasciitis refers to inflammation of the plantar fascia – a thick fibrous band that connects the heel to the front of the foot. The plantar fascia supports the arch of the foot and absorbs pressure. When it is inflamed or torn, putting pressure on the foot may result in sharp pain. Although the exact cause of plantar fasciitis is not clear, wearing inappropriate shoes, heavy work demands, obesity, running, and abnormal foot mechanics are some of the probable causes.
Symptoms of plantar fasciitis
- Pain in the bottom of the heel, extending into the arch of the foot.
- Intensity of pain may vary. It may be sharp or may feel like widespread soreness in the area surrounding the heel and the arch.
- Stabbing pain that occurs when you take your first steps in the morning. Pain normally decreases during the day with use of the foot, but may return after long periods of standing or when standing from a seated posture.
Who is at risk of plantar fasciitis?
While the cause of this condition is unclear, although there are factors that can increase risk of developing plantar fasciitis:
- Age – the condition is more common among those aged 40 – 60
- Flat feet, high arches, or tight calf muscles
- Obesity – extra pressure on your feet due to significant body weight
- Medical conditions such as arthritis
- Exercises that repeatedly impacts the plantar fascia such as running
- Standing for extended periods
- Wearing high-heeled shoes
What are the treatments available for heel pain?
Over 90% of those who have plantar fasciitis can improve within 10 months with the following remedies. They include:
- Stretching your calf muscles.
- Wearing supportive, sturdy, well-cushioned shoes (avoid sandals or flip flops that do not have a built-in arch support. Don’t walk with bare feet).
- Massaging the area.
- Limiting physical activity including prolonged standing.
- Taking over-the-counter nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen (always read package instructions).
- Losing weight.
Podiatrists can offer a wide range of treatments including recommendation/ issuing custom-made insoles, shoes inserts or night splints; physical therapy i.e. stretching and strengthening exercise plans; acupuncture; cortisone (steroid) injections or extracorporeal shockwave therapy (ESWT) to stimulate the healing process.
If you are suffering from ongoing heel pain, you should contact a podiatrist as they are best placed to help.
Remember – #podshealheels !
